|
By Dr. Jessica Warnecke PT, DPT, OCS 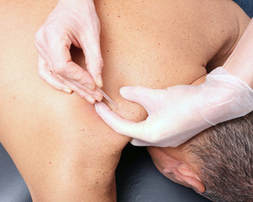 Dry needling is a term being used more often in today's western medical world, cross fit gyms, and therapy clinics around the country. Most people are familiar with acupuncture, but what exactly is the difference? Both use the same needles, both are geared at reducing pain. How do you choose one over the other, or do you possibly utilize both? The American Physical Therapy Association defines dry needling as "a skilled intervention that uses a thin filiform needle to penetrate the skin and stimulate underlying myofascial trigger points, muscular, and connective tissues for the management of neuromusculoskeletal pain and movement impairments. [It] is a technique used to treat dysfunctions in skeletal muscle, fascia, and connective tissue, and to diminish persistent peripheral nociceptive input, and reduce or restore impairments in body structure and function, leading to improved activity and participation.”
In other words, dry needling (DN) is often used when treating chronic musculoskeletal pain and trigger points (TrP). It is a Western Medicine technique and recent studies have shown positive results in reducing chronic neck and low back pain using dry needling techniques. In addition, multiple articles and systematic reviews report reduction of trigger point activity, decreased pain intensity, and increased patient self-report measures regarding function immediately, and up to 4 weeks, after dry needling techniques performed to neck, shoulder, back and hip muscles. Trigger points can occur from a build-up of toxic chemicals that the body is unable to remove following tissue trauma, muscle dysfunction, or an injury. Many people feel a “knot” with pain where a TrP is present. There are three types of TrPs: active, latent, and satellite. This categorization helps to understand the relationship between TrPs and symptoms they cause. Active TrPs present with spontaneous pain- no pressure or motion needed. Latent TrPs produce pain when pressure is applied. A satellite TrPs is present in the specific area of referred pain that radiates from an active TrP. Dry needling techniques are strategically utilized to target these trigger points and release them. The release restarts an inflammatory process in the body in order to flush out the noxious chemicals and help the muscle fibers reset to work properly. This allows pain to be suppressed and blocks the system that was causing the muscles to twitch out of sequence. This will help resolve pain, reduce muscle tension, and promote healing. In contrast to targeting trigger points, acupuncture is an Eastern Medicine technique in which needles are inserted into body meridians to treat certain physical, mental, and emotional conditions. The exact science behind how acupuncture works is still unclear. Some people feel it works by balancing energies, while others think it has a neurological effect. In acupuncture, the needles are inserted in a certain body Qi region and left for an extended period of time. With DN, the techniques are generally fairly quick and last from 5 seconds to a few minutes depending on which region of the body is being worked on. Acupuncture is a common practice for a select group of people; however, it is not one of the treatment options offered through physical therapy. So, although the needles are identical in both dry needling and acupuncture, the target points and needling techniques are different. Trigger Point Dry Needling is a valuable and can be an effective treatment for musculoskeletal pain. Certified physical therapists complete extensive training to incorporate dry needling with their knowledge of human anatomy and manual treatment techniques. If you have been suffering from muscle pain or limited mobility, talk with a physical therapist to see if dry needling is an appropriate option to help you heal.
1 Comment
Thanks for helping me understand that dry needling treatments would be strategically utilized to ensure that the trigger points are targeted and released. I guess I would consider trying this treatment for my left wrist, since it has been hurting for a week now. It might have been caused by typing for hours every day for the past couple of months.
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
Meet Your TherapistJessica has been in Austin, TX for the past four years. She grew up in Idaho and attended PT school at Idaho State University. She completed an Orthopaedic Residency and became a Board Certified Orthopaedic Clinical Specialist in 2016. Archives
February 2022
Categories
All
|

 RSS Feed
RSS Feed